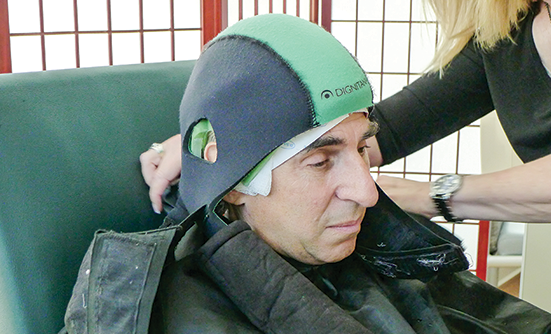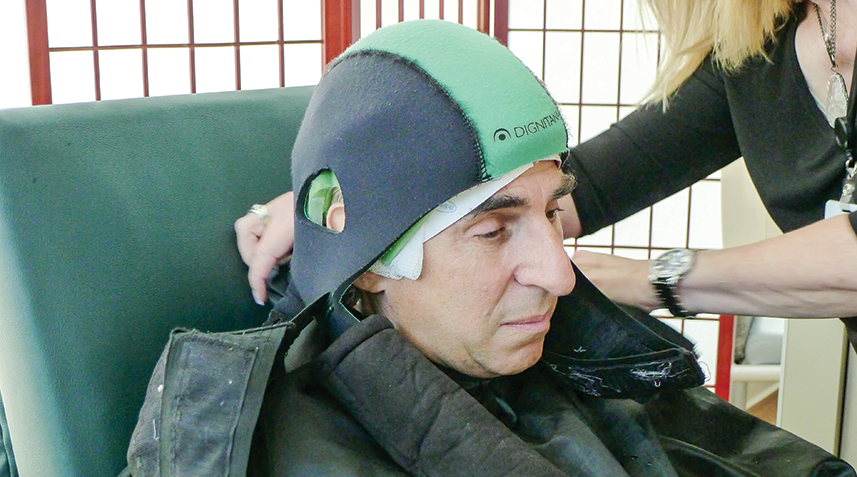
For Adrianne Frost, it wasn’t the ominous “you have cancer” diagnosis 2 years ago that took her breath away. It was the near certainty that the chemotherapy treatment required to save her life would leave her bald.
A new survey of patients with breast or ovarian cancer presented at ESMO 2017, the annual meeting of the European Society for Medical Oncology, showed that hair loss is among the most-dreaded side effects for patients undergoing cancer treatment. “Hair loss remains a persistent unresolved issue that is particularly difficult for patients at the start of treatment,” said Beyhan Ataseven, MD, from Germany, who presented the survey results.
The prospect of losing her hair hit Ms. Frost, 43, of San Antonio, TX, like a runaway freight train when she was told that she had breast cancer. “The diagnosis didn’t faze me as much as the certainty of losing my hair with the chemotherapy treatment,” recalls this real estate agent.
Finding a Remedy
Ms. Frost had heard reports that a scalp-cooling system had just been approved by the FDA. But the system was only available in few cancer centers where clinical trials were conducted. She decided this would not dampen her resolve to tunnel through the serpentine bureaucracy to get her cancer center to install the system in time for her first chemotherapy treatment. She distilled what could typically be a lengthy, 6-month ordeal into an intense, 6-week campaign.
“I made it my mission. It was actually very therapeutic,” she recalls of the mountain of paperwork and negotiations she had to spearhead. “It took my mind off what I was going through.” Ms. Frost became the first patient with breast cancer in the United States to use the system outside of clinical trials.
Maintaining Control
Allen Wasserman, a New York City attorney, was diagnosed at age 59 with stage IV gastric cancer that had spread to his esophagus and liver. An oncologist challenged Mr. Wasserman’s resolve to use scalp cooling: “What’s the big deal if you lose your hair?” his oncologist asked. Mr. Wasserman remembers taking a deep breath before he replied bluntly, “It means more to me than you think. Have you got a pair of scissors? I’ll take a snip of your hair, and see how you like it.”
Keeping up appearances has its advantages, especially in front of a jury. An anxious client who left the law firm in fear that Mr. Wasserman might not be able to represent him in court fueled his resolve to persevere with a scalp-cooling system.
“If you lose your hair, it’s a constant reminder that you will be treated differently,” Mr. Wasserman says. “I wanted to do what I could to retain some control of the situation.”
Weeks later, after a chemotherapy treatment session, Mr. Wasserman arrived at court to present a final argument. Surrounded by plaintiffs, judge, and jury, Mr. Wasserman recalls realizing that, “I knew how bad I felt, but I knew from the faces looking back at me that they didn’t know how bad I felt.” He won the case, for which he credits his courtroom skills, as well as his full head of hair.
HairToStay to the Rescue
Devastated by the news of an endometrial ovarian cancer diagnosis in 2016, Carla Thomas was doubly upset by the cost of a hair-loss remedy. The cost of a cooling system is typically $350 per infusion session.
To her rescue, and to the rescue of 500 patients to date, the nonprofit organization HairToStay has helped patients pay for the scalp-cooling systems, with subsidies up to $1,000. Founded in 2016, the organization has seen an increase in patients’ requests for support from 12 a month to 20 a week—a rate that is not sustainable without additional funding, according to Bethany Hornthal, Founder and CEO of HairToStay.
“The evolution of patients’ burden and their inability of paying have created a sense of urgency on our part,” she says. The organization is now aggressively soliciting help from hair salons and hair care manufacturers. They also helped Ms. Thomas to pay for her DigniCap system.
Hope for the Future
Scalp cooling is not a guarantee against hair loss. The systems’ effectiveness ranges from 30% to 80% of hair retention; it is not advised for patients receiving some types of chemotherapy. Manufacturers are looking for innovative technology to improve the systems’ overall outcomes.
Scalp-Cooling Systems
In July 2017, the FDA approved the use of the automated DigniCap Cooling System in any patient with solid tumors. It was first approved by the FDA in 2015 for women with stage I or II breast cancer to reduce hair loss from chemotherapy. The new approval was based on data showing that the DigniCap can also help patients with solid tumors in parts of their body other than the breast. The DigniCap is not approved for use in children and in some other patients. Another automated cooling system is the Paxman Scalp Cooling System, which was approved by the FDA in April 2017. With automatically controlled scalp-cooling systems, the cap is attached to a small refrigeration machine that circulates coolant, so the cap only has to be fitted once.
Scalp-cooling systems (or cold caps) are purchased by a cancer treatment center, and patients are charged for their use while receiving chemotherapy. The systems require patients to wear them before and after infusion, adding time to the procedure. The systems work by narrowing the blood vessels beneath the skin of the scalp, reducing the amount of chemotherapy medicine that reaches the hair follicles. Less chemotherapy reaching the follicles reduces the likelihood of hair falling out.
Recent studies show that women with early-stage breast cancer who used a scalp-cooling system were significantly more likely to keep at least some of their hair through chemotherapy.
Patient Resources
http://www.dignicap.com
http://www.hairtostay.org
http://www.wishcaps.com