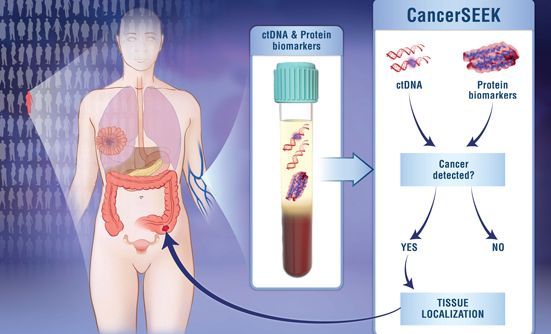
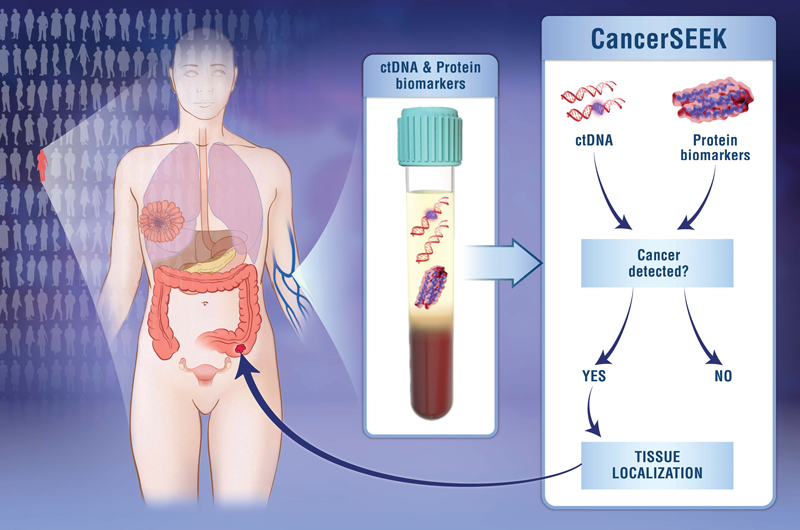
A new, simple blood test called CancerSEEK has the potential to change the way patients are being screened for cancer. This new blood test screens for 8 types of cancer, including breast, colon, liver, lung, esophageal, ovarian, pancreatic, and stomach cancers, from circulating DNA in the blood (Figure).1 The test also identifies 16 different types of cancer-related genomic mutations (changes), which may increase risk for certain cancer and can affect what type of medications are appropriate for a specific patient.
This noninvasive test may help to detect cancer in early stages, when treatment has the most chance to be successful.
Early Detection of Cancer Biomarkers
“This study is a very important step toward the development of a test for the early detection of cancer,” said Nickolas Papadopoulos, PhD, Professor of Oncology and Pathology, in a Johns Hopkins press release,1 who led the research that developed the test at Johns Hopkins Kimmel Cancer Center. He cautioned, however, that more studies are needed to confirm the accuracy of the test before it can be used by doctors, including primary care doctors.
CancerSEEK was evaluated in 1,005 patients with ovarian, liver, stomach, pancreatic, esophageal, colon, lung, or breast cancer. All cancers were in early stages, and had not spread in the body.
“The use of a combination of selected biomarkers for early detection has the potential to change the way we screen for cancer,” said Dr. Papadopoulos.1 The study’s findings were recently published in the journal Science.2 “Circulating tumor DNA mutations can be highly specific markers for cancer. To capitalize on this inherent specificity, we sought to develop a small yet robust panel that could detect at least one mutation in the vast majority of cancers,”1 said Joshua D. Cohen, an MD/PhD student at John Hopkins School of Medicine, and the first author of the article.
Tumor Types
Overall, the blood test detected cancer 70% of the time. Ovarian cancer was detected most accurately in 98% of cases; breast cancer was the least accurate, with 33% of cases diagnosed.
Ovarian, liver, stomach, pancreatic, and esophageal cancers, which currently have no screening tests available, had detection rates ranging from 69% to 98%. In addition, in 83% of patients, the CancerSEEK test was able to determine where the cancer originated.
“Besides detecting cancer, we were actually able to localize the cancer to one or two sites in the body. This is very important, because if this test is validated in future studies, once you find a signal that an individual may have cancer, the next question is where, and in what organ,” Dr. Papadopoulos said.
Although the test cannot screen for all types of cancer, these 8 types account for more than 60% of cancer-related deaths in the United States, the researchers say.2 The test may also be expanded to other cancers later on, but the researchers decided to limit the number of mutations and cancers tested to increase accuracy.
“If we are going to make progress in early cancer detection, we have to begin looking at it in a more realistic way, recognizing that no test will detect all cancers,” said Bert Vogelstein, MD, Co-Director of the Ludwig Center, Clayton Professor of Oncology and Howard Hughes Medical Institute investigator, in the press release.1
Specificity Is Key
This novel test differs from other molecular tests that analyze more cancer-driving genes that could be targeted by specific drugs, because its only purpose is to screen for cancer, with a more than 99% specificity for cancer.
“Very high specificity was essential, because false-positive results can subject patients to unnecessary invasive follow-up tests and procedures to confirm the presence of cancer,” said Kenneth Kinzler, PhD, Professor of Oncology and Co-Director of the Ludwig Center, in the press release.
The test also screened 812 healthy people, and only 7 of those had false-positive results, a very small percentage compared with other tests. Still, more work is needed to determine just how effective the test is at detecting early cancer. It is now being tested in people who have not been diagnosed with cancer.
Knocking on the Future’s Door
“Optimally, cancers would be detected early enough that they could be cured by surgery alone, but even cancers that are not curable by surgery alone will respond better to systemic therapies when there is less advanced disease,” said Anne Marie Lennon, MD, PhD, Director of the Multidisciplinary Pancreatic Cyst Program at Johns Hopkins, in the press release.1 The goal is to keep the cost of the test to less than $500 and to use it annually, along with other screening tests, such as mammograms and colonoscopies. Because a blood test is not invasive, it could be done by primary care doctors during routine annual blood tests.
“We would like to use it as a screening test for cancer. A simple test that everyone is willing to test,” Dr. Papadopoulos added. “We think that this type of test can change how we think about cancer, and put early detection as the main goal, and treating cancer as the second step.”1 “This test represents the next step in changing the focus of cancer research from late-stage disease to early disease, which I believe will be critical to reducing cancer deaths in the long term,” said Dr. Vogelstein.1
References
1. Johns Hopkins Medicine. Single blood test screens for eight cancer types. Press release. January 18, 2018. www.hopkinsmedicine.org/news/media/releases/single_blood_test_screens_for_eight_cancer_types.
2. Cohen JD, Li L, Wang Y, et al. Detection and localization of surgically resectable cancers with a multi-analyte blood test. Science. (Feb 23)2018;359:926-930.