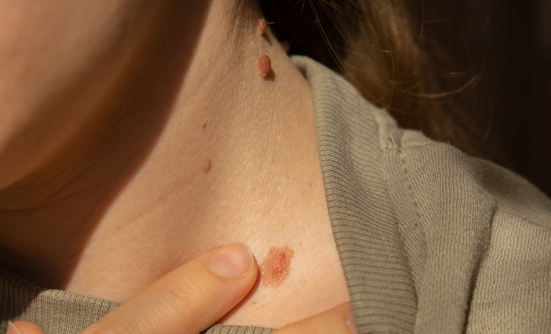
Melanoma is among the 3 most common types of skin cancer, along with basal-cell carcinoma and squamous-cell carcinoma: 1 in 50 Americans will have melanoma in their lifetime.
The American Cancer Society estimates that more than 3 million cases of skin cancer are diagnosed in the United States each year; of these, 73,870 were estimated to be new cases of melanoma in 2015. Melanoma is more likely to spread to nearby lymph nodes and to additional parts of the body than the other types of skin cancer, which complicates the patient’s treatment.
The incidence of melanoma is on the rise, especially among men older than 50 and women aged 15 to 29. With increased exposure to ultraviolet radiation from the sun and indoor tanning, melanoma has become the most common cancer among young adults aged 25 to 29.
How Melanoma Develops
Melanoma begins in the cells that produce the melanin pigment and are located in the top layer of skin. Melanoma can be found anywhere on the skin, but is especially common on the chest and back in men, and on the legs in women. Melanoma can also occur on the neck, face, eyes, mouth, genitals, and the anal area.
During the early stage (the radial growth phase), melanoma grows horizontally, staying within the upper layer of the skin. In the second (vertical) growth phase, melanoma begins to move into deeper skin layers, with an increased risk for spreading (metastasis) to other areas of the body. Melanoma cells may enter the lymph nodes or the bloodstream, allowing the cancer cells to spread to other organs.
Risk Factors
Exposure to ultraviolet rays (through sunlight, tanning beds, and sun lamps) is a major risk factor for melanoma, because of the damage caused to the DNA of skin cells. Other risks include:
- Moles/atypical moles: Individuals with inherited or atypical moles (dysplastic nevi) have a very high lifetime risk for melanoma; moles present at birth increase the risk for melanoma
- Fair skin, freckling, and light hair: The risk for melanoma is much higher for whites than for African Americans, and for whites with red or blond hair, blue or green eyes, or fair skin that freckles or burns easily
- Family history or personal history of melanoma: 10% of all patients with melanoma have a family history of the disease
- Weakened immune system
- Increasing age
- Gender: Before age 45, the risk for melanoma is higher in women; after age 45, the risk is higher in men
- Xeroderma pigmentosum (a rare condition that affects the skin cells’ ability to repair DNA damage)
Symptoms of Melanoma
The most important warning sign is a new spot on the skin, or a spot that looks different from other spots or moles, or a spot that is changing in size, shape, or color. Melanoma is diagnosed by examining skin tissue that is removed by a biopsy or surgery.
The ABCDE rule. A good way to remember the signs of melanoma is the ABCDE rule, which means:
- A = Asymmetry: one half of a mole or birthmark doesn’t match the other half
- B = Border: the mole has irregular, ragged, notched, or blurred edges
- C = Color: the color of the mole is not the same all over and may have shades of brown or black
- D = Diameter: the mole is larger than 6 millimeters
- E = Evolving: the mole is changing in size, shape, or color
Other warning signs for melanoma include:
- A sore that does not heal
- Spread of pigment from the border of a mole into surrounding skin
- Redness or a new swelling beyond the border
- Change in sensation (itchiness, tenderness, or pain)
- Change in the surface of a mole (scaliness, oozing, bleeding, or the appearance of a bump or a nodule)
Molecular testing of a tissue sample can help to identify mutations (changes) in the BRAF gene; people with a BRAF mutation are at an increased risk for melanoma.
Treatment
Surgery
Surgery is typically the main treatment option for melanoma, and often is the only treatment necessary to cure early-stage melanoma. Surgical procedures include wide excision, which removes the melanoma along with a measured area of normal tissue as a precaution; lymph node mapping and sentinel lymph node biopsy to detect melanoma cells in nearby lymph nodes; and lymph node dissection to remove groups of lymph nodes in the area near the primary melanoma.
Immunotherapy
Immunotherapy seeks to stimulate the body’s own immune system to attack melanoma cells. Interferon-alfa and interleukin-2 are types of man-made proteins that help immune system cells attack cancer. One type of immunotherapy includes immune checkpoint inhibitors, which help destroy cancer cells.
New immune checkpoint inhibitors currently being used to treat advanced melanoma are the PD-1 inhibitors Keytruda (pembrolizumab) and Opdivo (nivolumab), and the CTLA-4 inhibitor Yervoy (ipilimumab).
In January 2016, the FDA approved the first combination of PD-1 inhibitors, Opdivo plus Yervoy, for the treatment of patients with advanced melanoma or melanoma that cannot be removed by surgery.
In October 2015, the FDA approved the first oncolytic virus, Imlygic (talimogene laherparepvec, also known as T-VEC), a new type of immunotherapy for recurrent (returning) melanoma that can’t be removed surgically. Imlygic is a virus that is injected into the tumor to kill cancer cells.
Targeted Drugs
In recent years, doctors have uncovered genetic mutations that make melanoma cells different from normal cells. Approximately 50% of all patients with metastatic melanoma have BRAF mutations, which cause melanoma cells to grow and divide more quickly than normal cells. This discovery has led to the development of drugs that attack cells with certain mutations.
Drugs for melanoma that target BRAF mutations are called BRAF inhibitors and include Zelboraf (vemurafenib) and Tafinlar (dabrafenib). Targeted drugs for melanoma that target MEK proteins are called MEK inhibitors and include Mekinist (trametinib) and Cotellic (cobimetinib).
Combining a BRAF inhibitor with a MEK inhibitor has been shown to shrink tumors for a longer period of time than when either drug is used alone. Therefore, using 2 drugs in combination—Mekinist plus Tafinlar or Cotellic plus Zelboraf—is an attractive treatment option for patients with advanced melanoma who have BRAF mutations.
Several drugs that target other abnormal genes or proteins are being studied in clinical trials, including Nexavar (sorafenib), Avastin (bevacizumab), Votrient (pazopanib), Afinitor (everolimus), Gleevec (imatinib), and Tasigna (nilotinib).
Chemotherapy/Radiation Therapy
Chemotherapy is not as effective for melanoma as for other cancers and is used primarily to relieve stage IV melanoma symptoms. Radiation therapy has been shown to reduce the risk for relapse (returning disease) in several situations.
Clinical Trials
New treatments for melanoma are being evaluated on a daily basis in clinical trial research. In addition to speaking with the oncology team, patients can learn about available clinical trials through the National Institutes of Health at www.clinicaltrials.gov.
Patient Resources
American Cancer Society
https://www.cancer.org/cancer/melanoma-skin-cancer.html
Melanoma International Foundation
http://melanomainternational.org
Melanoma Research Foundation
www.melanoma.org
Skin Cancer Foundation
www.skincancer.org