To download this article as a PDF, see the link below.
CPS1334
In April 2018, patient advocates from North America, South America, and the European Union met in Berlin, Germany, to discuss the challenges faced by people living with multiple myeloma. In this second annual Global Patient Leadership Council (GPLC) Multiple Myeloma Roundtable, which was sponsored by Takeda Oncology and moderated by CONQUER, patient advocates shared their experiences with multiple myeloma and brainstormed about practical ways to address unmet needs that would benefit patients and their families around the world.
After sharing many different aspects of their experiences with multiple myeloma, the patient advocates were clear that, because everyone’s individual journey is unique, learning and communicating openly with the healthcare team is critical. Research studies show this, too. Patients who share their expectations and preferences with their healthcare teams may have better health outcomes.1
This publication summarizes the roundtable discussion for patients, caregivers, and the doctors and nurses who are a part of the global multiple myeloma community. It is divided into 5 sections that summarize key learnings related to the following topics:
- Learning Starts at Diagnosis
- Treatment Choices for a Complex Condition
- Sharing in Decision-Making
- Caring for the Caregiver
- Building a Global Multiple Myeloma Community.
Learning Starts at Diagnosis
What Is Multiple Myeloma?
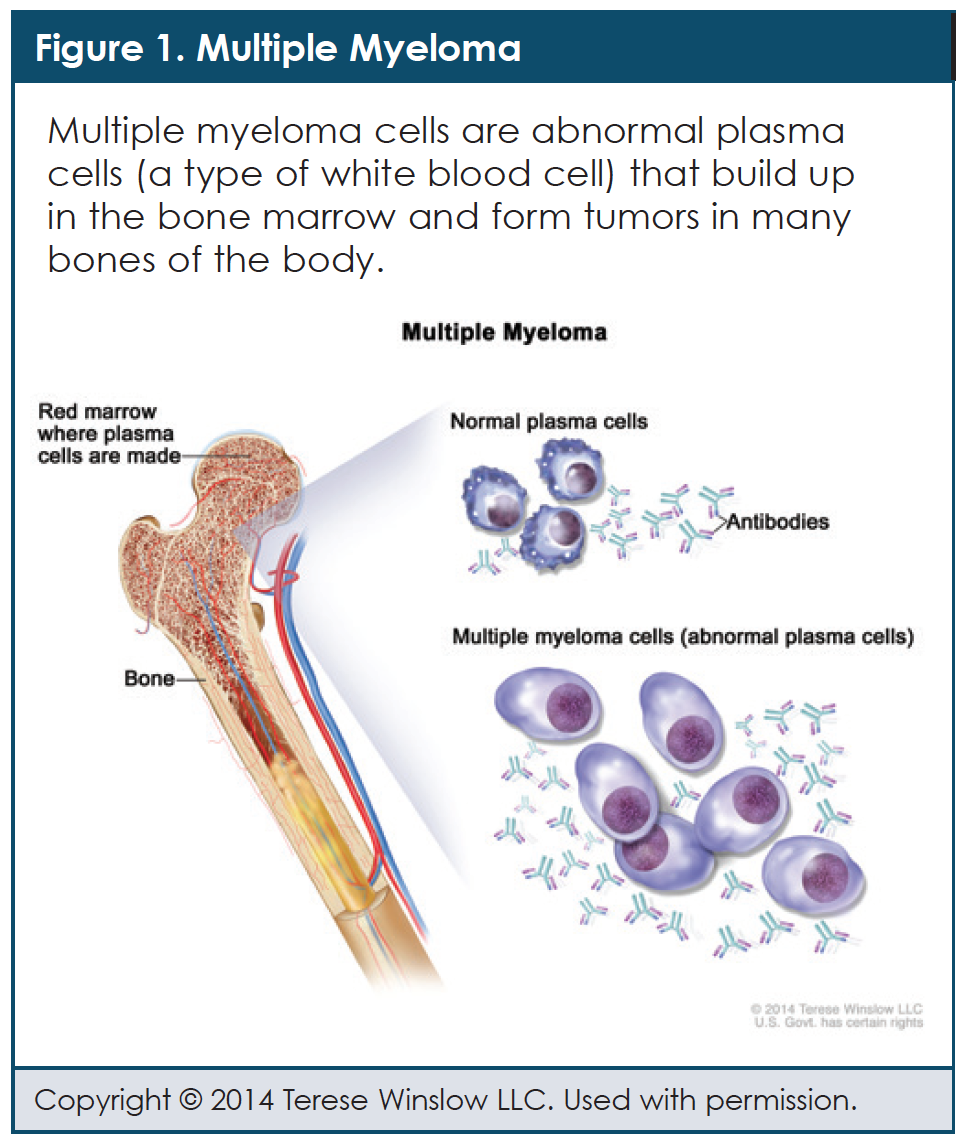
Before reviewing insights related to living with multiple myeloma, it helps to briefly summarize the condition. In multiple myeloma, white blood cells called plasma cells, which are found in the bone marrow, become cancerous or malignant (Figure 1).2 These cancerous plasma cells are called myeloma cells. Growth of myeloma cells often occurs in bones where marrow is very active, such as the spine, skull, rib cage, pelvis, shoulders, and hips. The word “multiple” is used because the disease can occur in several areas of bone. On scans, multiple myeloma can look like a tumor (1 disease site) or can result in several different patches of bone loss.2
As it grows, multiple myeloma can weaken bones and prevent the bone marrow from forming blood cells. This means that patients can have anemia (low levels of red blood cells), thrombocytopenia (low levels of platelets), or leukopenia (low levels of normal white blood cells).2 People with multiple myeloma can also experience pain, bone fractures, weakness, fatigue, bruising, or bleeding, and can have a tough time fighting infections. Multiple myeloma can also result in high levels of abnormal monoclonal proteins, called monoclonal immunoglobulins, that can damage kidneys and other organs.2
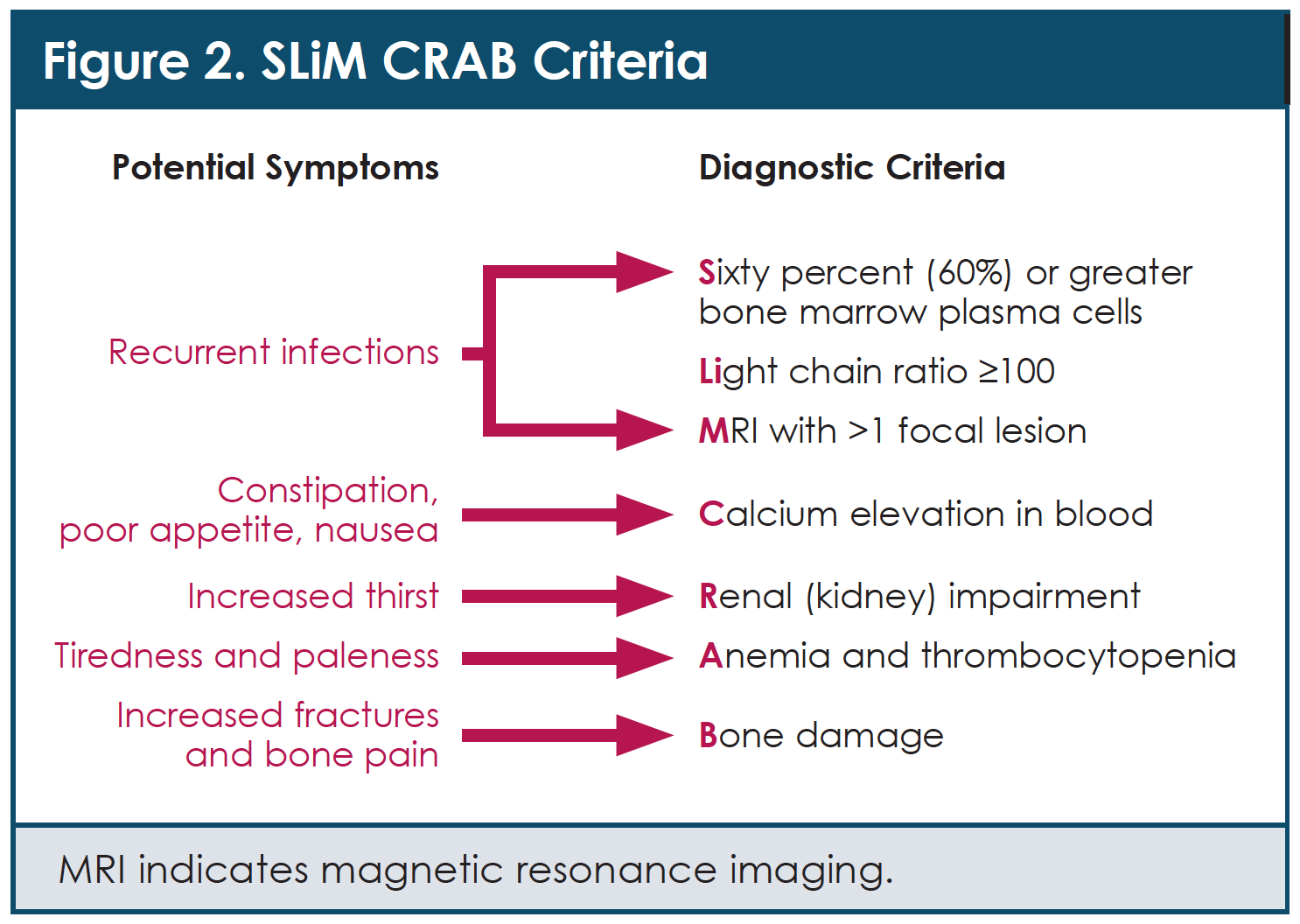
The acronym “SLiM CRAB” can be used to remember some of the common symptoms and signs (diagnostic criteria) that are observed at the time of diagnosis in people with multiple myeloma (Figure 2).3
Significant Progress in Multiple Myeloma Treatment
Many patients with multiple myeloma can lead long and productive lives after being diagnosed.4 According to the International Myeloma Foundation, more than 229,000 people are living with multiple myeloma worldwide.2 Specifically, in the United Kingdom and the United States, statistics show that approximately half of patients with multiple myeloma will survive for at least 5 years after their diagnosis.5,6
With a better understanding of the disease and as more effective therapies have been developed, overall survival rates have increased significantly in multiple myeloma, according to a study of more than 1000 patients diagnosed with the disease between 2001 and 2010.7 Of note, statistics from this time frame do not capture the impact of new treatments that have been introduced since 2010 or the effect of continued improvements in the safety of stem-cell transplantation.
One of the biggest challenges in multiple myeloma is access to treatment. Patient advocates who participated in the GPLC Multiple Myeloma Roundtable recognized that many patients worldwide cannot access the therapies necessary to treat their disease. Cost, availability, and whether insurers and national health system payers are willing to cover treatments are often barriers to patient access.8 These advocates’ organizations are dedicated to ensuring that patients have access to all of the medications that they need.
Potential for Delayed Diagnosis in Multiple Myeloma
As in other rare diseases with symptoms that can be vague, it is not unusual for patients with multiple myeloma to see several different medical specialists before a diagnosis is made. Most primary care physicians, orthopedists (bone specialists), and nephrologists (kidney specialists) do not immediately think of multiple myeloma when they initially see an older patient with back pain, fatigue, or kidney problems. Multiple myeloma is uncommon; the average primary care physician is likely to see fewer than 10 patients with the disease throughout his or her career.9
Studies that have been conducted to better understand this delay in diagnosis have shown that bone pain is, by far, the most common reason for patients with multiple myeloma to seek medical care.9,10 Findings from a large, global, prospective, observational study (INSIGHT-MM) showed that almost one-third (34%) of 1000 patients with multiple myeloma from around the world sought medical care because of bone pain.10 The next symptoms—weakness and fatigue—were mentioned as the reason to seek care by 13% of patients, whereas kidney problems prompted patients to seek treatment in only 6% of cases.10 If the diagnosis of multiple myeloma is delayed, cancer has more time to grow (ie, it may be more advanced) and myeloma-related symptoms can be more severe, which can have a negative impact on the quality of life of patients.
“My husband’s diagnosis was delayed for more than 6 months because he had a blood test and the doctor, his general practitioner, found anemia. In fact, he was anemic because it was multiple myeloma.”
—Viorica Cursaru
“People whom I have known have gone to chiropractors and were told, ‘It is just a back problem.’ It has taken several months, if not years, before their bone pain was associated with multiple myeloma.”
—Yelak Biru
Because early diagnosis is so critical, patient advocates feel it is important to raise awareness of multiple myeloma and its symptoms. In particular, there should be more educational programs for primary care physicians to help them recognize the early signs of the disease and understand the tests they can use to make a diagnosis. Other healthcare providers who need to be better informed are medical specialists who see patients who have come to them because of unexplained bone pain or kidney problems.
Learning About Multiple Myeloma
After being told that they have multiple myeloma, patients and their families are rightly alarmed and stressed. Most want to know the likely physical, emotional, social, and financial impacts the disease will have on them and their loved ones, as well as their prognosis. Doctors who treat people with cancer, including multiple myeloma, need to recognize patients’ level of understanding and state of mind as they help prepare them for the road ahead.
As the shock of a cancer diagnosis wears off, it is important for patients with multiple myeloma to realize that, unlike with many other illnesses and cancers, their journey is often long-term. Multiple myeloma is a disease with periods of disease remission and relapse.11 People with multiple myeloma often receive different types of treatment in sequence (ie, “lines” of treatment) over their lifetime.12
Because multiple myeloma often requires a long-term approach, patients and their healthcare team can talk about different options and plan the journey. In most instances, patients have time to learn about the disease, find the best doctors to treat them, talk about treatment options, and prepare themselves (and their families, caregivers, coworkers, and friends) for the next steps.
Patient advocates who participated in the GPLC Multiple Myeloma Roundtable shared their personal insights and experiences related to learning more about multiple myeloma, as well as their ideas for others who are newly diagnosed with the disease.
Step 1: Prioritize accurate and up-to-date information
There are many sources of information and advice about multiple myeloma, particularly online. Because searching the Internet is easy, many patients and their families start there. However, patient advocates note the need to be cautious about sources; patients’ personal experiences that are shared online are not as reliable as information collected through robust research, including clinical trials. In addition, new information about multiple myeloma becomes available at a fast pace. Internet-based information needs to be up-to-date, clear, and accurate. Patients should focus on information that is reported by experts and reputable organizations.
“There is too much information out there. Finding reliable information is the challenge. Referring
to patient organizations
is a great first step.”
—Yelak Biru
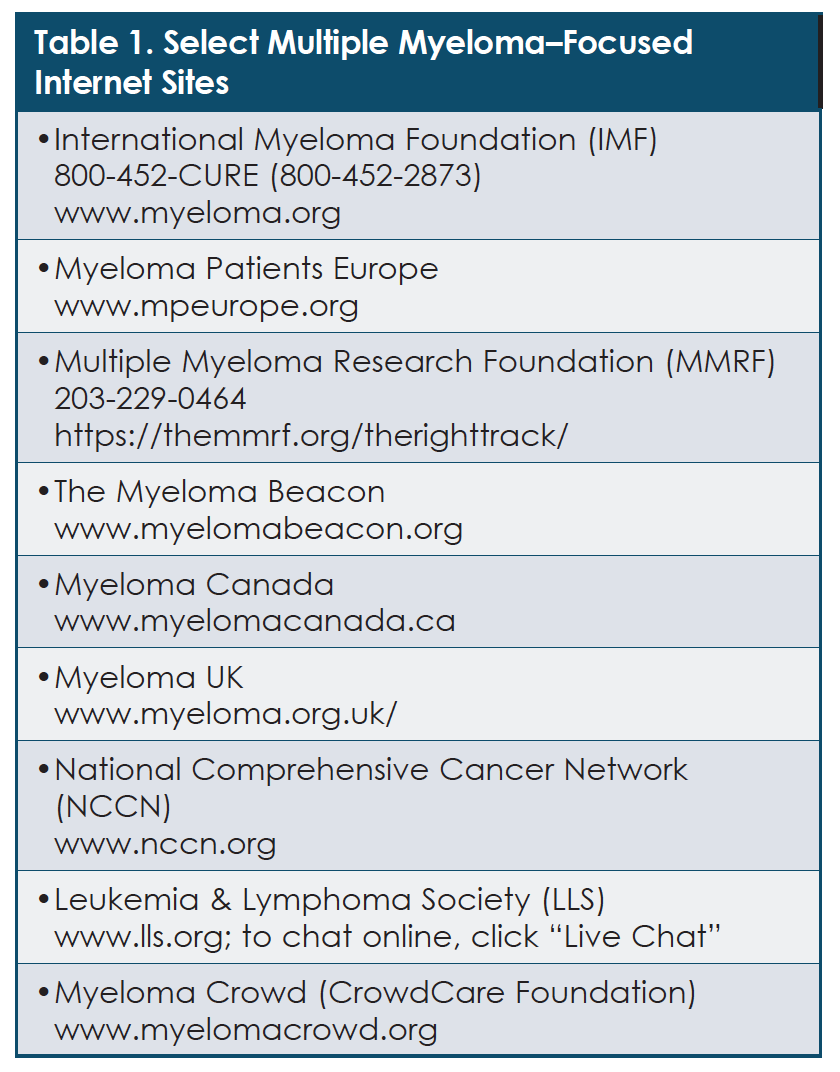
Which websites are best? The patient advocates believe that patient organizations offer trustworthy resources, as well as support for people with multiple myeloma. Pharmaceutical companies who make treatments for patients with multiple myeloma also have valuable educational resources and support programs. Table 1 provides a select list of multiple myeloma–focused Internet sites that were discussed during the Roundtable, including links to patient organizations dedicated to supporting the needs of people with multiple myeloma. The patient advocates noted that these free, reliable, and supportive websites give patients the chance to connect and learn. Doctors and nurses should also refer patients and their caregivers to support groups or patient organizations that can help them obtain answers to their questions, gain insight and support, and ultimately feel more comfortable talking with the healthcare team.
Step 2: Assemble your healthcare team
The patient advocates highlighted the need for all patients to feel comfortable with the doctors, nurses, and other healthcare professionals who provide their cancer care. Whether this team of professionals is small or large, patients with multiple myeloma should receive the best quality of care available.
“You need a healthcare team that works together. They all need to know about each other, and it is the patient’s job to keep everyone informed about his or her medications and about decisions that have been made.”
—Yelak Biru
Each patient with multiple myeloma will have different preferences and needs, which means they need to find a cancer care team that is a good fit for them. Healthcare providers should work with each patient to find the best solutions for his or her medical needs and respect the patient’s requests for second or even third opinions.
Whether patients live in a rural village, a suburban town, or a large city, it is important for them to consider meeting with a multiple myeloma specialist. These doctors often practice in a specialty center or “Center of Excellence,” which may be located within a larger hospital or university. Multiple myeloma specialists provide focused care, and often have access to the newest diagnostic tests and treatments, including clinical trials.13
Nurses also play a key role in the healthcare team. In addition to providing direct medical care, they are often able to discuss complex information with patients and caregivers. Nurses are more likely to use terms that are clear and easy to understand. They also advocate for the patient who is experiencing complications or side effects. Some patients are not comfortable sharing side effect information with their doctor; therefore, nurses can be an important “point of contact.” If necessary, nurses can also refer patients to other professionals who can provide psychosocial support, financial assistance, or other services.
Whenever possible, multidisciplinary healthcare teams should work together to decide which treatment choices are most appropriate at each point in the patient’s journey. Multidisciplinary teams include several different types of cancer care providers (Figure 3), each of whom have unique perspectives. Whether this team is large or small, the members should work together, communicate often, and keep the patient’s needs and wants the top priority when making recommendations.
Key Points
- For a growing number of patients, multiple myeloma is a chronic condition. Patients do not need to panic—there is time to learn and absorb needed information. Patients should consider asking family members or friends for help.
- After diagnosis, one of the first things patients should do is find a multiple myeloma specialist or go to a Center of Excellence, if available. When possible, patients should ask for second opinions from multiple myeloma specialists if they wish to be treated closer to home.
- It is easy to overload on poor-quality information about cancer using the Internet, including social media sites. Patients should prioritize learning about multiple myeloma from trustworthy and up-to-date information sources, such as those listed in Table 1. The patient’s healthcare team is there to offer information and support. Patients with multiple myeloma are tasked with finding the best team available in their country, and using the team’s knowledge and experience to learn as much as possible.
- Patients should not be afraid to ask questions of doctors and healthcare providers. They should write down their most pressing questions and the answers that are given.
- Patients with multiple myeloma should connect with other patient and caregiver mentors using free support services that are available online, via telephone, and in local hospitals.
Step 3: Connect with other patients with multiple myeloma
As with many illnesses that affect a small number of people, patients with multiple myeloma and their caregivers look to each other for information, empathy, and support. Learning about the experiences of others with the disease is often a great source of support for patients who are diagnosed with the same condition or cancer.
One way to help people with multiple myeloma connect with each other is to participate in a support group, either through a patient organization or through physicians’ offices or hospitals. Another way is through mentor-matching programs, such as the Leukemia & Lymphoma Society’s Patti Robinson Kaufmann First Connection Program (www.lls.org/support/peer-to-peer-support), and My Mentor Connections, a mentoring initiative sponsored by Takeda Oncology for patients and caregivers in the United States (www.mymentorconnections.com or 844-482-6818).
Using these free programs, patients with multiple myeloma can be connected with a patient or caregiver mentor. These mentors are people who are living with multiple myeloma or caring for someone with the disease and who have been trained to support others. In general, mentors speak from personal experience about their journey. Some hospitals and universities with cancer centers may also have support groups and programs that match patients (and caregivers) with other patients (and other caregivers) who have experience dealing with similar situations.14 Patient advocates continue to develop initiatives such as these mentorship programs, as well as other solutions, for patients with multiple myeloma. Always be sure to get your medical advice from trained professionals. It is important to discuss these topics with your healthcare team.
Treatment Choices for a Complex Condition
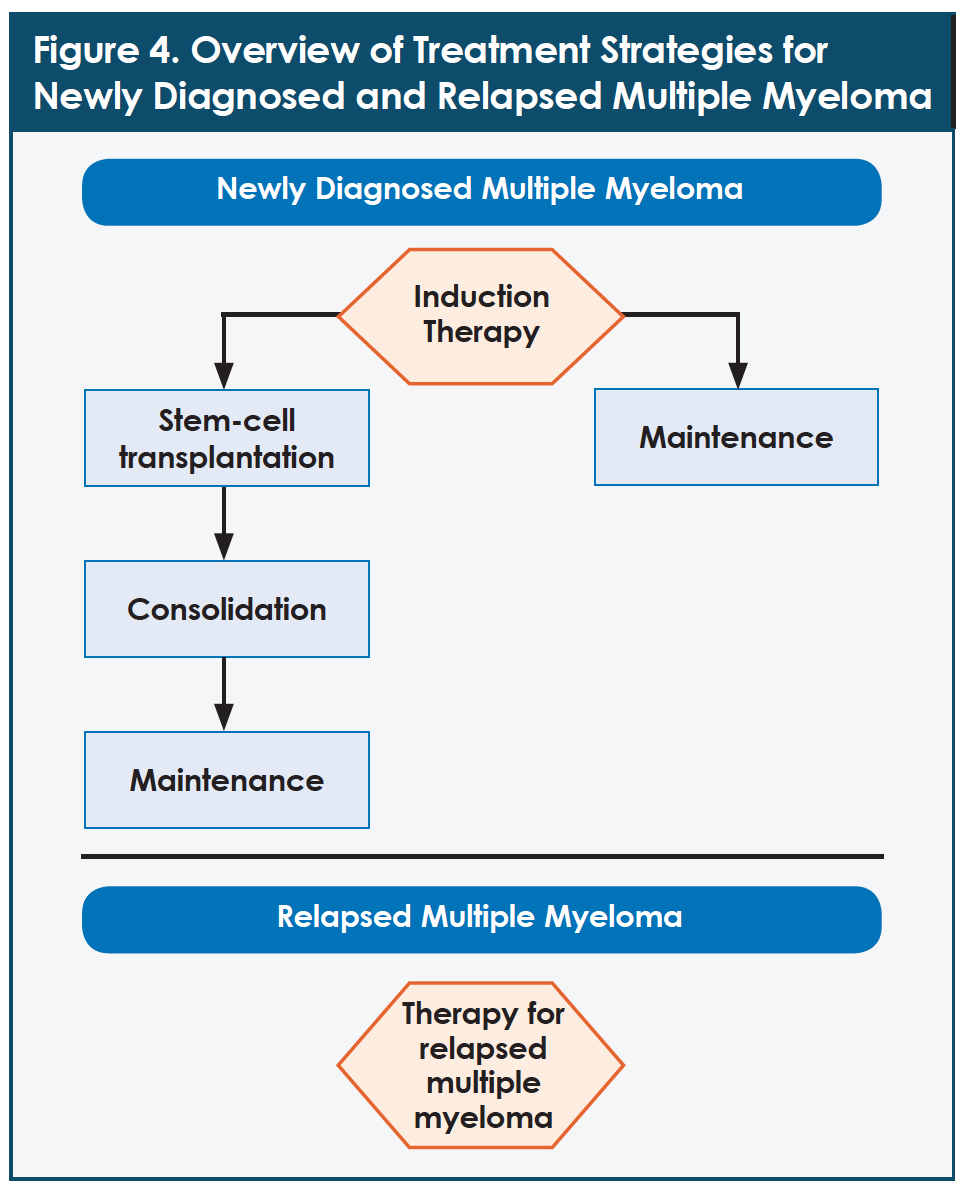
Based on educational materials provided by the National Comprehensive Cancer Network (NCCN), a not-for-profit alliance of 27 leading cancer centers in the United States, Figure 4 provides a simplified overview of the treatment approaches that can be considered for a patient with multiple myeloma at the point of diagnosis and at relapse.15 Of note, some treatment regimens contain 3 drugs (triplet regimens), whereas others contain 2 drugs (doublet regimens). Some drug treatments are used during the induction phase of treatment, whereas other drug treatments (and stem-cell transplant) are used during the consolidation phase of therapy. (An in-depth discussion of these terms is beyond the scope of this article. However, free educational materials provided by the NCCN offer patients and their caregivers a valuable overview of these topics and many others.15)
Key Points
- There are many treatment options for patients with multiple myeloma. Patients typically receive several “lines” of treatment in sequence throughout their journey with the disease.
- Use of combinations of medications is common in multiple myeloma. Studies have shown that use of 3 medications (triplet regimens) can be more effective than combinations of 2 medications (doublet regimens).16
- Two treatment paths are important in multiple myeloma based on the patient’s ability to undergo stem-cell transplantation. For some patients, induction therapy is followed by a stem-cell transplant, which is then followed by consolidation and maintenance therapy. For other patients, induction therapy is followed by continuous drug therapy.
- For some patients with multiple myeloma, use of maintenance therapy (medication given to maintain good results of previous treatment) offers improved outcomes, when available.
- Clinical trials offer another option for patients with multiple myeloma. Ask your doctor if clinical trials are available and if you are able to participate.
For many patients with multiple myeloma and their families and caregivers, the fact that there are several treatments available to fight their disease is a source of great hope. At the same time, the need to learn about and choose from among so many treatment options can result in confusion or anxiety.
It is important to note that the availability of treatment options varies from one country to the next, depending on the country’s healthcare system. As a result, some patients have limited treatment choices, which can also be a source of anxiety.
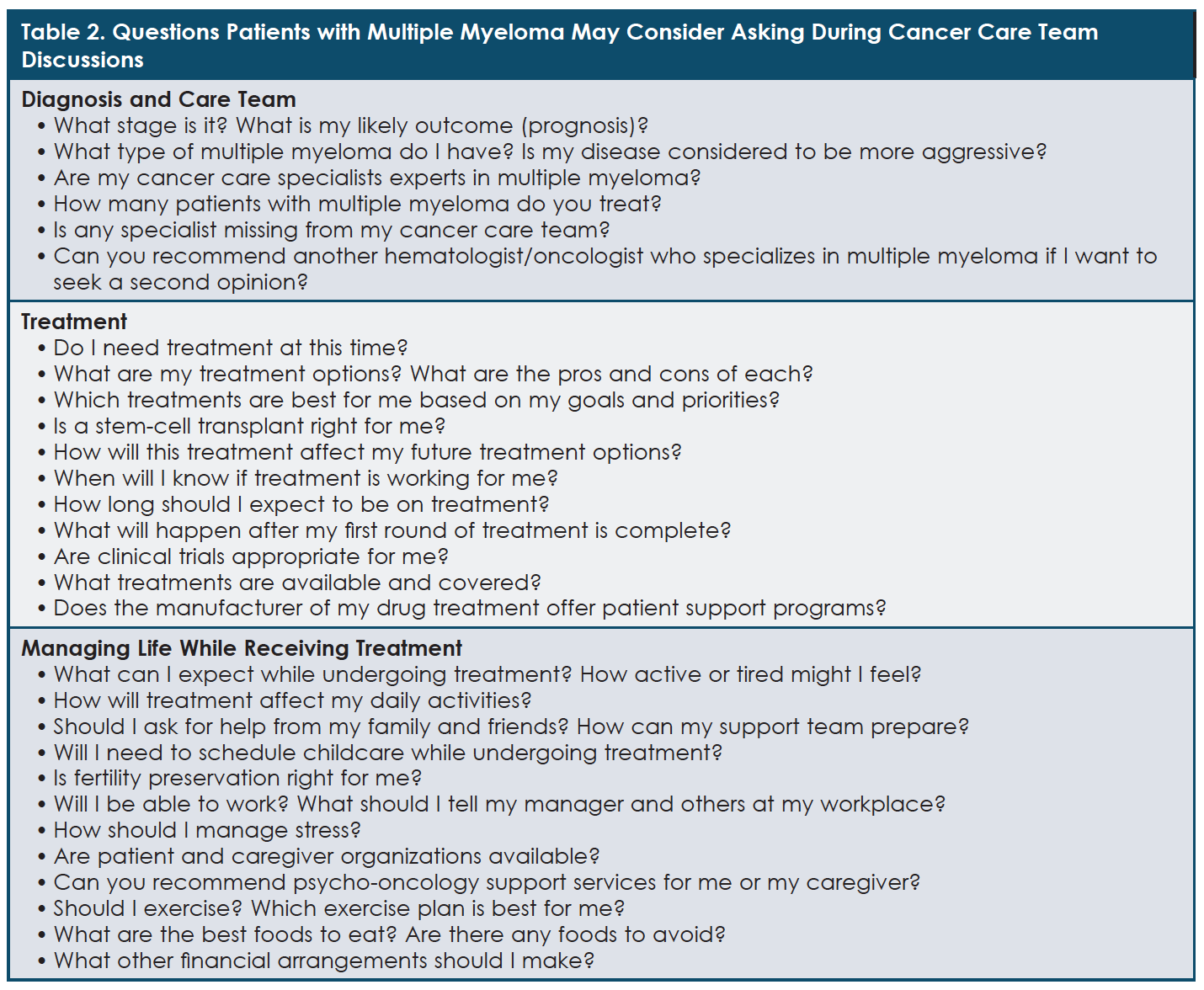
Patients with multiple myeloma cannot be expected to understand which treatment options are best for them, which sequence of available therapies is optimal, or which treatments will ensure good quality of life. Their cancer care team is responsible for sharing information about each relevant option, guiding them through decisions, and advising them when new decisions need to be considered. However, this does not mean that patients should be passive. Table 2 lists questions that patients with multiple myeloma may want to ask their cancer care team.17
Sharing in Decision-Making
Each patient living with multiple myeloma has different goals they want to achieve. One individual may want or need to continue working every day, whereas another may wish to retire or quit working to spend time with family or travel. A patient’s goals may also change over time. No matter what patients’ personal goals are, they and their caregivers need to talk about them with the healthcare team and revisit these goals throughout their journey.
The Roundtable participants believe that, even though most patients who are newly diagnosed are not experts in multiple myeloma, their opinions matter and should guide treatment choices when more than one option is available. What is the best treatment approach for an individual patient with multiple myeloma? Who decides what “best” really means? What role can the patient play?
“Caregivers need care as well.”
—Yelak Biru
Key Points
- lthough doctors are experts in multiple myeloma, patients are experts when it comes to their needs and desires. The patient’s needs, values, and preferences matter; his or her voice must be a part of the conversation, if they choose to be involved.
- Patients and their caregivers should do their best to make sure that their cancer care team offers treatments that reflect the patient’s values and preferences.
The term “shared decision-making” really means mutual information-sharing. The multiple myeloma care team should help patients understand the decisions they are facing, and patients should be able to help providers understand their needs, values, and preferences about these decisions.18 Ideally, patients with multiple myeloma and their doctors and nurses then come to an agreement about the treatment plan.18 Although taking a more active role may seem scary to some patients, resources are available to help, including lists of questions to consider (Table 3).19
Caring for the Caregiver
Patients with multiple myeloma find it helpful or necessary to have support from a caregiver. Caregiver support may range from driving the patient to and from doctor visits or making meals, to becoming a partner in the process of researching and understanding disease information, talking through hopes and fears, and making treatment decisions.20
Key Points
- Many local and national resources are focused on providing help to people with cancer and their caregivers. In addition to friends and local community services (eg, churches, food banks, transportation, home care providers), there are many national organizations that can help.
- Cancer caregivers need and should receive help throughout their journey with their loved one. Asking for help and accepting help when it is offered is not a sign of weakness or failure.
- Self-care is not selfish; caregivers who take care of themselves are better caregivers.
- Although people who care about the patient and the caregiver want to help, they may not always know what to say or do. Caregivers may need to tell them what specific types of help are needed.
- It is helpful to distribute requests among caregivers, delegating different tasks to different friends and family members.
Because caregiving can be stressful, it is critical for caregivers to take time for themselves and care for their own needs, especially if they have health problems of their own. Caregivers who skip their own doctors’ visits, eat and sleep poorly, stop exercising, and cannot find time to relax and recharge find it hard to remain strong and optimistic for their loved one.21
It is well-documented that the physical and emotional stress associated with caring for a loved one with cancer can be a lot to handle.20 For almost all caregivers, this role is new and different. The dynamics of the relationship between the caregiver and the patient with multiple myeloma may change. It is very normal for caregivers of people with cancer to feel confused, sad, tired, anxious, guilty, angry, lonely, and stressed.20,21
The Caregiver Action Network offers 10 useful tips for caregivers22:
- Seek support from other caregivers. You are not alone!
- Take care of your own health to be strong enough to take care of your loved one.
- Accept offers of help. Suggest specific things people can do for you.
- Learn how to talk effectively with doctors.
- Caregiving is hard work. Take breaks!
- Watch for signs of depression and get professional help if you need it.
- Be open to new technologies to help you care for your loved one.
- Update and organize medical information.
- Get legal documents in order.
- Give yourself credit for doing the best you can. This is a tough job!
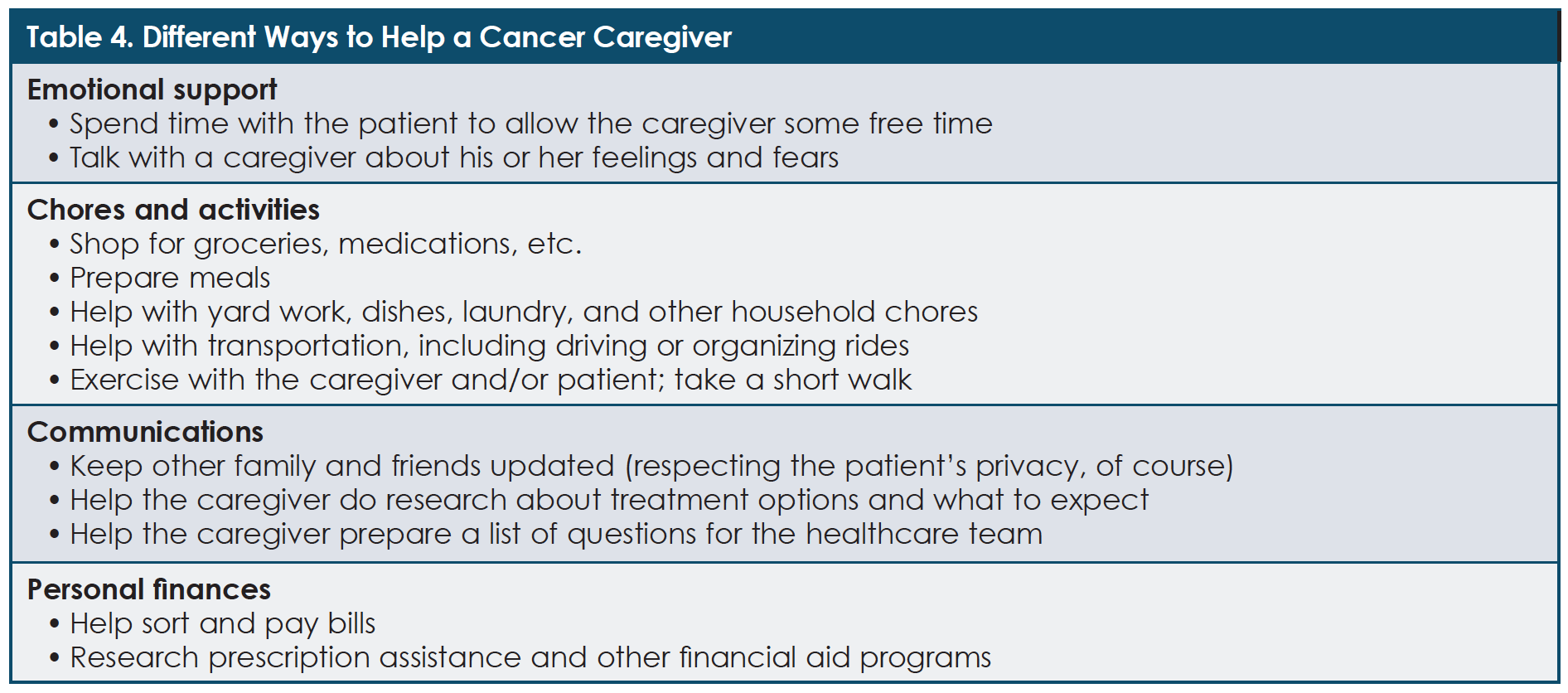
Table 4 provides some strategies for helping cancer caregivers.20 There are also numerous organizations that can provide support to caregivers, including CancerCare (www.cancercare.org), the Family Caregiver Alliance (www.caregiver.org), and Caregiver Action Network/Help for Cancer Caregivers (www.caregiveraction.org; www.helpforcancercaregivers.org). Myeloma UK (https://www.myeloma.org.uk/help-and-support/support-for-carers/) also has information on its website designed specifically for caregivers.
Key Points
- Data collected in clinical trials and data collected in real-world settings are different. It is important for patients and their caregivers to participate in all types of research.
- Participating in clinical trials is not the only way that people with multiple myeloma can advance scientific understanding and the development of new treatments. By volunteering their time and insights in a survey or observational study, patients can feel satisfied and proud that they have helped others with the condition.
Building a Global Multiple Myeloma Community
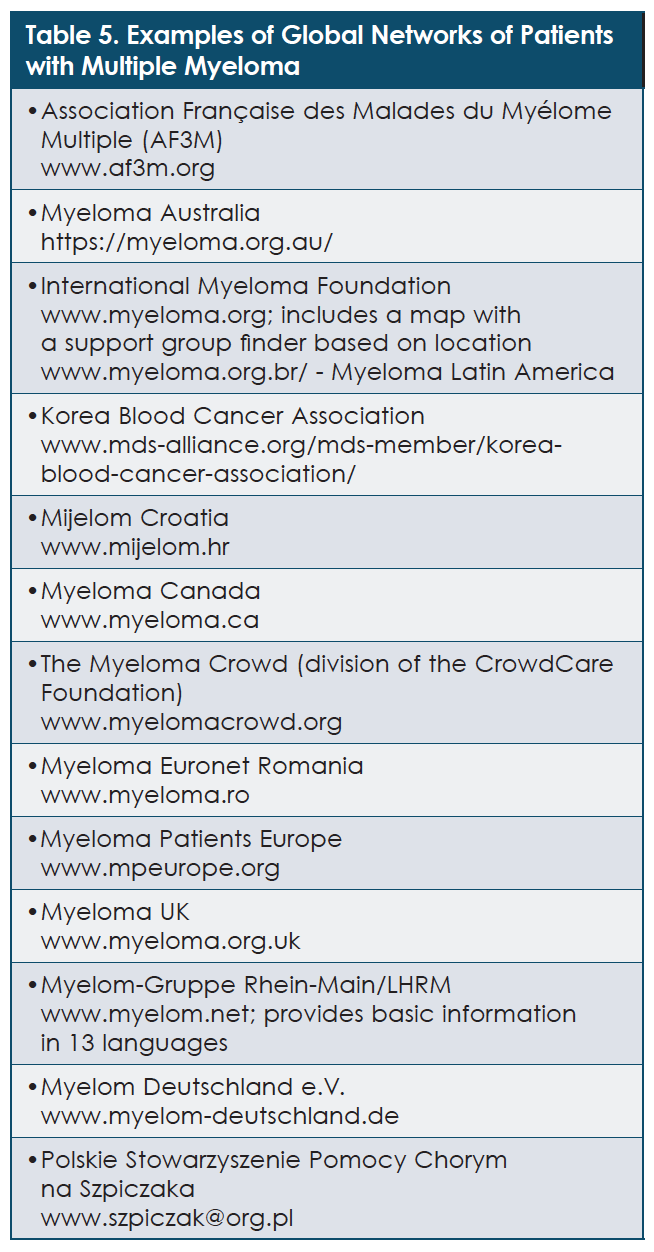
For patients with multiple myeloma around the globe, it is rewarding and valuable to belong to a community of people who can share experiences, ideas, and insights. Knowing that social media channels and other websites can offer valuable opportunities for interaction and support, multiple myeloma advocates have created specific resources for patients in many languages. Table 5 provides examples of national and regional websites that patients and their caregivers can use to find information about multiple myeloma and connect with others.
Clinical Trials and Patient Registries
Participating in research efforts is another way for patients with multiple myeloma worldwide to learn about each other and to advance scientific understanding. Most people know that clinical trials of medications and other interventions for patients with multiple myeloma are available, and that clinical trials are very important. In contrast, many people are not aware of observational studies, which include patient surveys and registry studies, or the important ways in which these research efforts can enhance clinical trial data.
Clinical trials do not always reflect the way care is provided to people who live with multiple myeloma and are treated outside a clinical trial setting. Clinical trials provide a narrow perspective, typically comparing one treatment with another during a specific treatment phase, and do not provide better understanding of long-term outcomes. In addition, as the patient advocates in the Roundtable noted, not all patients with multiple myeloma have access to clinical trials.
For patients who do not wish to participate in clinical trials, or who do not have access to them, registries (or observational studies) and patient surveys provide a great opportunity to give back and learn about the experiences of others living with multiple myeloma. Patients with multiple myeloma who participate in registries share their experiences regarding all different types of treatment, which helps multiple myeloma doctors better understand real-world experiences and outcomes, as well as patients’ concerns and preferences.
Observational studies, such as INSIGHT-MM,10 which is sponsored by Takeda, provide important insights into treatment patterns, patient preferences, and long-term outcomes. Other studies may be funded by patient organizations, government agencies, or your individual cancer center.
To learn more about how to find and participate in registries, patients with multiple myeloma can ask their physicians or explore programs offered by patient organizations.
References
- Hughes TM, Merath K, Chen Q, et al. Association of shared decision-making on patient-reported health outcomes and healthcare utilization. Am J Surg. 2018;216:7-12.
- International Myeloma Foundation. What is multiple myeloma? www.myeloma.org/what-is-multiple-myeloma. Accessed October 21, 2018.
- Managing Myeloma. International Myeloma Foundation. International Myeloma Working Group (IMWG) Updated Criteria for the Diagnosis of Multiple Myeloma. www.google.com/url?sa=t&rct=j&q=&esrc=s&source=web&cd=14&ved=2ahUKEwjOp8iio77eAhUhjoMKHXp9BpkQFjANegQ IChAC&url=http%3A%2F%2Fwww.managingmyeloma.com%2Ftools%2Fupdated-criteria-for-diagnosis%3Ftask%3Ddownload.file%26format%3Draw%26dlid%3D1011&usg=AOvVaw2qqla7JAviwy1pzx3Pw5fW.
- International Myeloma Foundation. Are you newly diagnosed? www.myeloma.org/are-you-newly-diagnosed. Accessed October 21, 2018.
- Cancer Research UK. Myeloma: survival. www.cancerresearchuk.org/about-cancer/myeloma/survival. Accessed October 21, 2018.
- National Cancer Institute SEER Program. Cancer stat facts: myeloma. https://seer.cancer.gov/statfacts/html/mulmy.html. Accessed October 8, 2018.
- Kumar SK, Dispenzieri A, Lacy MQ, et al. Continued improvement in survival in multiple myeloma: changes in early mortality and outcomes in older patients. Leukemia. 2014;28:1122-1128.
- Lawrence L. Global burden of myeloma increasing, access to treatments lacking. Cancer Ther Advisor. www.cancertherapyadvisor.com/multiple-myeloma/multiple-myeloma-global-burden-access-treatment-lacking/article/775072/. Accessed October 24, 2018.
- Goldschmidt N, Zamir L, Poperno A, et al. Presenting signs of multiple myeloma and the effect of diagnostic delay on the prognosis. J Am Board Fam Med. 2016;29:702-709.
- Boccadoro M, Usmani SZ, Chari A, et al. A global treatment standard in multiple myeloma remains elusive despite advances in care over 15 years: first results from INSIGHT MM, the largest global prospective, observational multiple myeloma study. Poster presented at: 23rd Annual Meeting of the European Hematology Association (EHA); June 14-17, 2018; Stockholm, Sweden. Poster PS1300.
- Osterweil N. Multiple myeloma: from palliative care to chronic therapy?— treatment advances edge disease toward curable status. ASCO Reading Room. www.medpagetoday.com/reading-room/asco/multiple-myeloma/57193. Accessed October 24, 2018.
- Cancer.net. Multiple myeloma: types of treatment. www.cancer.net/cancer-types/multiple-myeloma/types-treatment. Accessed October 9, 2018.
- Elrod JK, Fortenberry JL Jr. Centers of excellence in healthcare institutions: what they are and how to assemble them. BMC Health Services Res. 2017;17(suppl 1):425.
- Gordon A. Myeloma lessons: hey, hey, I’m a mentor! The Myeloma Beacon website. https://myelomabeacon.org/headline/2016/09/15/myeloma- lessons-hey-hey-im-a-mentor/. Accessed October 11, 2018.
- NCCN Guidelines for Patients®: Multiple Myeloma, 2018. www.nccn.org/patients/guidelines/content/PDF/myeloma.pdf. Accessed October 24, 2018.
- Durie B, Hoering A, Abidi MH, et al. Bortezomib with lenalidomide and dexamethasone versus lenalidomide and dexamethasone alone in patients with newly-diagnosed multiple myeloma without intent for immediate autologous stem cell transplant (SWOG S0777): a randomised, open- label, phase 3 trial. The Lancet. 2017;389(10068):519-527.
- Faiman B, Gleason C. How to talk with your health care team about what is best for you: shared decision making for patients and caregivers. www.myeloma.org/sites/default/files/images/SlidesAndAudioForVideos/lwm_shareddecisionmaking_faimangleason.pdf. Accessed December 16, 2018.
- Kane HL, Halpern MT, Squiers LB, et al. Implementing and evaluating shared decision making in oncology practice. CA Cancer J Clin. 2014;64:377-388.
- Agency for Healthcare Research and Quality. Clinically localized prostate cancer: deciding what is best for you. https://effectivehealthcare.ahrq.gov/decision-aids/prostate-cancer/23.html. Accessed October 11, 2018.
- National Cancer Institute, National Institutes of Health, US Department of Health and Human Services. Caring for the Caregiver. NIH publication 14-6219. www.cancer.gov/publications/patient-education/caring-for-the-caregiver.pdf. Accessed October 9, 2018.
- Help for Cancer Caregivers. Practical matters: getting caregiver help. www.helpforcancercaregivers.org/topics/practical-matters. Accessed October 9, 2018.
- Caregiver Action Network. 10 tips for family caregivers. https://caregiveraction.org/resources/10-tips-family-caregivers. Accessed October 9, 2018.
In Memoriam: Aldo Del Col
Aldo Del Col, Co-founder of Myeloma Canada, was committed to ensuring that patients with multiple myeloma understood their condition and had access to the medicines they needed. His direct impact on the quality of life of people living with multiple myeloma outshines his recent passing and will continue to encourage others with myeloma to advocate for each other. We are grateful to Aldo for his contributions to this article, and know that his passion for helping others will continue to touch all who read it.
MAT-USO-NON-19-00097