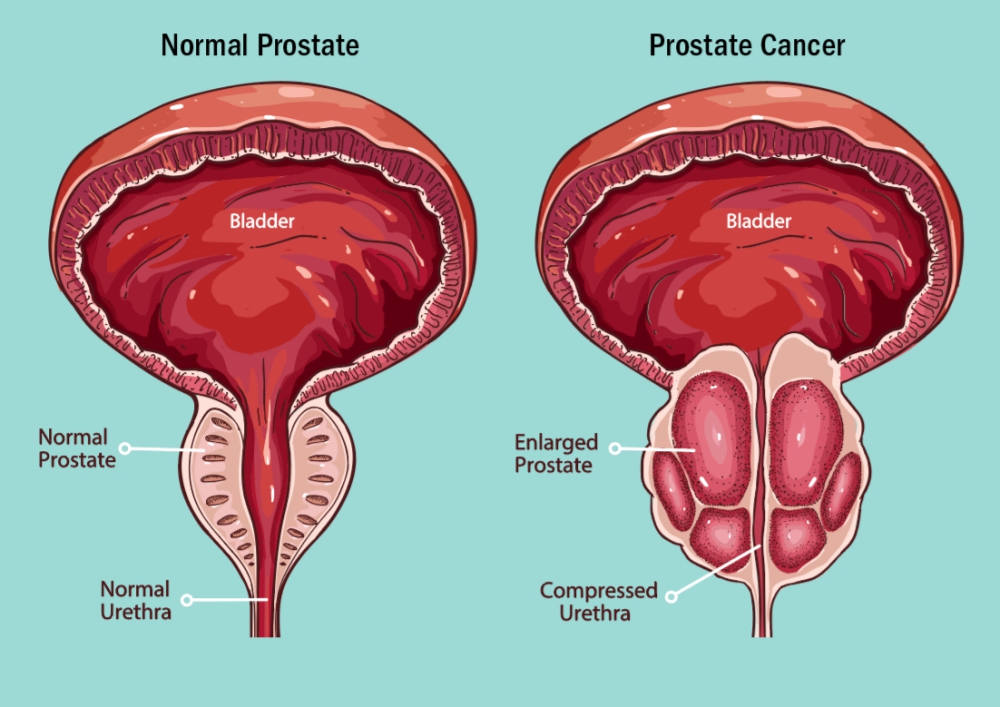
Men’s cancers, including prostate, bladder, testicular, and penile cancers, are often misunderstood by patients and by healthcare providers.
The earlier these cancers are found, the better the man’s chances of successful treatment and survival, so understanding these cancers is crucial for any man diagnosed with one of these cancers.
At a recent Oncology Nursing Society conference, Joan Livingstone, BScN, RN, OCN, from the Karmanos Cancer Center in Detroit, Michigan, discussed the symptoms, diagnosis, and self-care strategies related to prostate cancer that can make a big difference for patients and their caregivers.
The Symptoms of Prostate Cancer
Prostate cancer is the most common cancer in American men, except skin cancer, and is the second leading cause of cancer death in American men (after lung cancer). According to the American Cancer Society, about 268,490 men will die of prostate cancer in 2022. And about 13 of every 100 men will be diagnosed with prostate cancer at some point in their lives.
Most men with prostate cancer are at least 50 years old (the average age at diagnosis is 66), and most men with prostate cancer will have some of the following symptoms:
- Difficulty starting urination
- Weak or interrupted urine flow
- Frequent urination, especially at night
- Difficulty emptying the bladder completely
- Pain or burning during urination
- Blood in the urine or semen
- Pain in the back, hips, or the pelvis that doesn’t go away
- Painful ejaculation.
Screening and Diagnosis
According to Ms. Livingstone, African-American men are at increased risk for prostate cancer and should begin annual prostate-specific antigen (PSA) screenings at age 45. Men of other ethnic groups can begin screening at 50, unless they have a family history of prostate cancer, in which case they should also start screening at age 45.
Patients whose PSA level is elevated will be referred to a urologist and will likely have other tests, but just as important as PSA screening is a rectal exam (called digital rectal exam), Ms. Livingstone said.
Although the PSA testing is used to evaluate a man’s risk for prostate cancer, this test is not perfect, because there could be several reasons for elevated PSA levels. Some of the main reasons are:
- An enlarged prostate gland that is benign and is often seen in older men (called PBH, or benign prostatic hyperplasia)
- Older age often causes the PSA levels to go up but have no relation to cancer
- Prostatitis, an infection or inflammation of the prostate gland that can also increase the PSA levels.
Some medications can also increase the risk of prostate cancer. Despite these reasons, the PSA test is a good way to indicate that a man may have prostate cancer and should have additional testing to investigate that possibility or rule out prostate cancer.
Imaging for prostate cancer diagnosis can be done through an ultrasound of the prostate, or through an MRI of the pelvis, focusing on the prostate.
When a doctor suspects prostate cancer, a diagnosis is typically made through a prostate biopsy that is guided by ultrasound, in which 2 small pieces are taken from the prostate gland.
Treatment
Ms. Livingstone discussed the approach to prostate therapy.
Surveillance. The treatment of a patient with prostate cancer will vary, depending on the patient’s risk factors and his prognosis. For men with very low-risk prostate cancer and a life expectancy of 10 years or more, active surveillance is preferred to surgery or medications.
“Active surveillance is active monitoring of the patient’s prostate cancer, with an expectation to intervene with curative intent when or if the cancer progresses,” Ms. Livingstone said.
According to the American Cancer Society, these men should have a PSA test every 6 months, and a rectal exam at least every 12 months. Prostate biopsy and MRI should not be done more often than every 12 months.
Prostatectomy. Surgery to remove the prostate is called prostatectomy, and is recommended for patients with high-risk or very high-risk prostate cancer who have a life expectancy of 10 years or more.
Radiation is another common treatment choice for men with prostate cancer.
Medications. The combination of drug therapy with surgery, or radiation therapy with hormone therapy called androgen-deprivation therapy (or ADT)—which involves drugs that reduce a man’s testosterone level in the body—is another common treatment option for men with prostate cancer.
Treatment Side Effects
It is important to take vitamin D and calcium when using androgen-deprivation therapy, because these types of drugs can increase the patient’s risk of fractures and osteoporosis.
Overall, the treatment for prostate cancer can have significant side effects for men, but there are therapies that can be used to minimize or prevent those side effects.
For example, the SpaceOAR hydrogel procedure can minimize the side effects of radiation therapy, by creating a buffer between the rectum and the prostate.
This procedure can help patients to maintain sexual function, while also decreasing their chance of having bowel control problems. Therefore, patients should always discuss such options with their doctor.
Patient Resources
American Cancer Society
www.cancer.org/cancer/prostate-cancer.html
Centers for Disease Control and Prevention
www.cdc.gov/cancer/prostate/basic_info/index.htm
National Cancer Institute
www.cancer.gov/types/prostate/patient/prostate-prevention-pdq