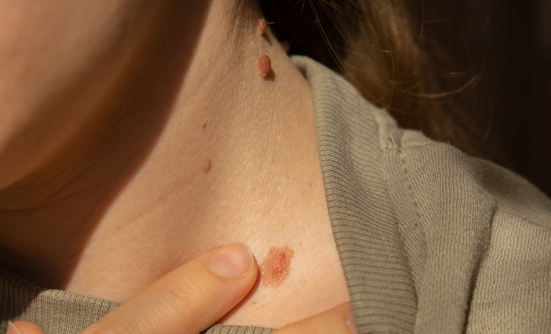
Skin cancer is the most common type of cancer in the United States, with 3.5 million patients diagnosed each year. According to the American Cancer Society, approximately 76,100 patients will be diagnosed with melanoma this year, with about 1,000 more men than women. Close to 10,000 deaths were caused by melanoma in 2014, with twice as many deaths in men than in women. Men tend to have a higher mortality rate, because late detection in men means the melanoma is found at a later growth stage.
Melanoma is not just skin cancer, which is the title of my recent book, to emphasize this misconception about melanoma. It is a type of skin cancer, but not the garden variety, such as squamous-cell or basal-cell skin cancers. More often than not, these types of skin cancer are excised, and you no longer need to worry about them. However, if melanoma is not caught early, it can spread and become life-threatening.
Fortunately, melanoma grows on the outside of our bodies (with the exception of rare types of mucosal and ocular melanoma), where it can be readily seen by the naked eye. When it is caught early and removed properly with a wide excision, you can probably feel confident that it won’t come back.
However, melanoma often misbehaves and can be misread by the pathologist. Therefore, it is wise to have a dermatopathologist do the pathologic analysis, and/or to get a second opinion.
Risk Factors
What causes melanoma? It is unlikely that melanoma is hereditary; the culprit is likely ultraviolet (UV) radiation from the sun or from tanning lamps/beds. Less than 4% of melanoma is familial, and it is often found in families that have many moles or atypical moles, or a predominance of red hair and fair skin. This appearance can indicate the P16 gene, which is the main gene that has been linked to melanoma.
When melanoma is genetic, there are usually 2 or more close blood relatives who have melanoma. The likelihood of it running in families is often attributed to families that spend their summers tanning at the shore, or spend their winters in sunny places. A tan is still a relished skin feature in our society, and remains the main reason behind the increased number of melanoma and skin cancer cases.
Prevention
Melanoma and skin cancer can be prevented by covering yourself with protective clothing, seeking shade, wearing sunscreen, and staying out of direct sunlight during the peak hours of 10 AM to 4 PM.
Avoiding tanning salons is imperative, because using tanning beds can increase your risk for melanoma by 75%. Prevention is a tough row to hoe, and it may take many years of strategy to raise awareness about the dangers of UV light exposure.
Shallow-depth (or in situ) melanoma is unlikely to spread; however, deeper melanomas can spread to vital organs, such as the lungs, liver, or brain, just like any other cancer.
Skin exams are important for finding melanoma early, and you can do it just as easily as your doctor. After all, you know your skin better than your doctor who sees many patients daily.
Treatment Options
Patients who have melanomas that measure 0.76 inches or deeper usually receive a sentinel node biopsy to see if the melanoma has spread to their lymph nodes. If there is 1 or more nodes that test positive for melanoma, the patient is considered to have stage III melanoma.
Sadly, we have no great choices for adjuvant therapy yet, and watching and waiting is often the only choice for patients in this situation. If the melanoma progresses to stage IV, then choices emerge for some promising therapies.
The treatment of melanoma has taken center stage in cancer research, and it is high time. After 40 years of little or no progress in treatment, we now have therapy choices.
We don’t have a cure for spreading melanoma quite yet, but patients are certainly living longer, and with higher-quality lives. If we can figure out how to catch all melanomas early, when they are curable, or prevent them from happening at all, that would be an astounding feat!
Patient Resources
Patients with Stage IV Melanoma Speak Out
http://melanomainternational.org/events-webinar/patient-experience-video/#.VYhZG2TF9xs
Skin Exam
http://melanomainternational.org/melanoma-facts/examine-your-skin/#.VYhZLWTF9xs
Patient/Caregiver Moderated Forum
http://www.melanomaforum.org/