In 2013, actress Angelina Jolie announced her decision to undergo a bilateral mastectomy after learning that she carried the BRCA1 gene mutation (alteration), which is strongly associated with increased risk for breast cancer and ovarian cancer. Her decision sparked the public’s interest in the role of genetic testing and preventive surgeries, especially for people who have family histories of certain cancer types.
The so-called Angelina effect has highlighted the benefits of genetic testing, but testing is not without its own risks and limitations. At the Women’s Survivors Alliance SURVIVORville 2015 meeting, Sara Lewis, MS, LCGC, Hereditary Cancer Clinic, Vanderbilt-Ingram Cancer Center, discussed the key issues that arise before people pursue the option of genetic testing.
Benefits of Genetic Testing
According to Ms. Lewis, the benefits of genetic testing include:
- Identifying people at high risk for cancer in families with a known genetic mutation
- The possibilities of earlier detection and start of prevention strategies
- Relieving the anxiety of not knowing whether you’re at high risk for cancer
“My patient isn’t just you,” said Ms. Lewis. “It’s your family too. This affects everybody.”
The Drawbacks
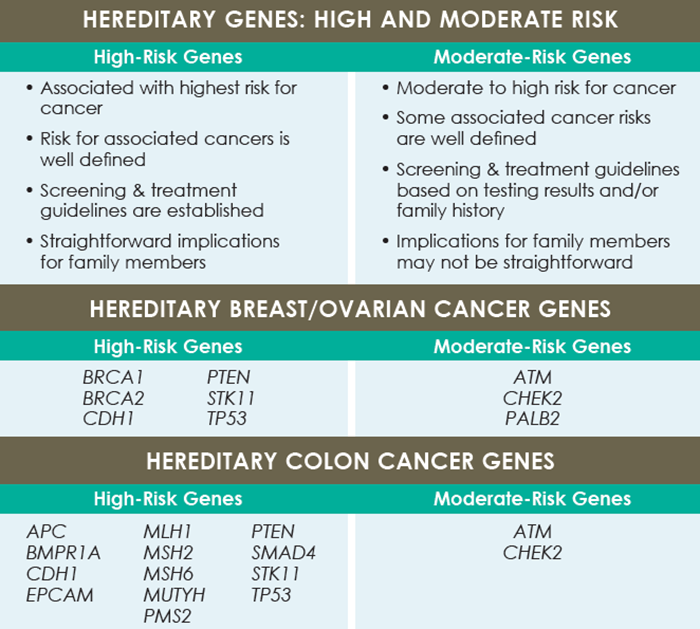
Some genes are well-known to increase the risk for cancer, but the risk of other genes is not always known. The Table explains the difference between high-risk and moderate-risk genes for developing cancer.
Genetic testing does not detect all genetic alterations, and people are at risk for nonhereditary cancer. “Most cancer occurs randomly due to environmental exposures, such as alcohol or smoking,” Ms. Lewis said. “A lot of people who know a family member who died of a certain cancer don’t know where it started. It’s important to get information about where the cancer started, not where it spread, and then ask them what treatment they went through.”
Insurance Coverage
Patients should also consider the cost of genetic testing, which varies depending on the gene being tested, ranging from a few hundred dollars to a few thousand dollars. “Most insurance companies cover the cost of genetic testing if an individual meets certain criteria,” Ms. Lewis said.
Under the Affordable Care Act (ACA), genetic counseling and genetic testing are considered as preventive care. Health insurance plans must pay for genetic counseling and genetic testing for people who meet certain criteria, such as women who don’t have symptoms of a BRCA genetic alteration but who have a family history of BRCA.
The ACA also states that health coverage applies to nongrandfathered private health insurance policies, and that people must meet certain family history criteria that were established by the US Preventive Services Task Force to qualify for genetic testing.
Ms. Lewis noted that the ACA does not cover the total cost of genetic counseling or testing in men, in people with a family history of Lynch syndrome (which is associated with colon, endometrial, ovarian, stomach, pancreatic, and other cancers) or with other hereditary cancer syndromes, or in women who have already been diagnosed with cancer.
People who want to get genetic testing should get more information from their health insurance providers about their coverage, she said.
The Genetic Information Nondiscrimination Act
The Genetic Information Nondiscrimination Act prohibits health insurance plans from using genetic information to determine insurance coverage eligibility and the amount of premiums. The act also prohibits health plans from requiring genetic testing for coverage eligibility and from employers making employment or job status decisions based on genetic testing results.
Ms. Lewis explained that although the Genetic Information Nondiscrimination Act provides certain protections, the act does not include protections in life insurance, disability insurance, and long-term care insurance, and it excludes members of the military. The act also does not require insurance companies to pay for genetic testing.
Patient Resources
National Society of Genetic Counselors
http://nsgc.org/
NCI Cancer Genetics Services Directory
http://www.cancer.gov/about-cancer/causes-prevention/genetics/directory














