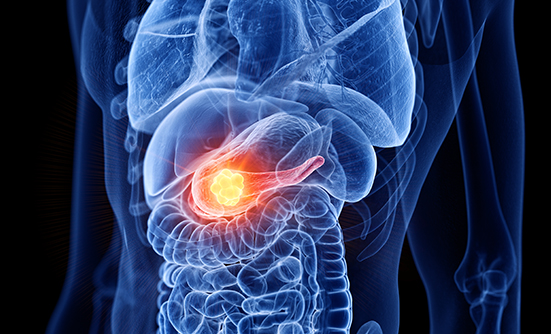
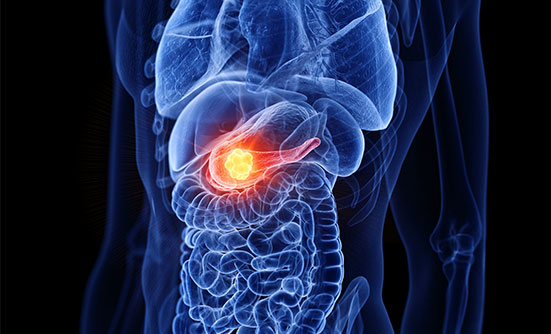
Pancreatic cancer has the potential to become the second leading cause of cancer deaths in the United States by 2020, but it is already wreaking havoc on the lives of thousands today. According to the National Cancer Institute, in 2019, an estimated 56,770 people will be diagnosed with pancreatic cancer, and an estimated 45,750 people will die of the disease.1
A recent high-profile diagnosis that has drawn international attention is that of Alex Trebek, host of Jeopardy, who announced in early May 2019 that he had stage IV (metastatic) pancreatic cancer (that has spread to other parts of the body). Trebek is the latest in a long line of celebrities who have faced this type of cancer, including Patrick Swayze, Michael Landon, and Dizzy Gillespie, all of whom died of metastatic pancreatic cancer within a few months to years after diagnosis (Steve Jobs had a less-common type of pancreatic cancer).
Although Trebek recently shared the good news that his tumors were shrinking with treatment, the reality surrounding pancreatic cancer is often grim.
The cure rate for stage I pancreatic cancer (meaning early disease) is anywhere from 20% to 40%, but when it is diagnosed in the later stages, that rate drops significantly. At advanced or metastatic stage (stage IV)—the stage that Trebek is facing—the cure rate is much smaller, and the 5-year survival rate is just 9%, meaning that about 10 of 100 individuals with stage IV pancreatic cancer will survive at least 5 years.1
Obviously, the key to successfully fighting pancreatic cancer is diagnosing it as early as possible, but how to do this is not so obvious.
The Challenge of Early Diagnosis: Vague Symptoms
There is no single red flag that alerts patients and/or their doctors to the possibility that someone has pancreatic cancer. Typically, patients who will eventually be diagnosed with this cancer first head to the doctor for vague abdominal pain. Because this is such a general and not specific symptom, doctors appropriately believe that the patient is dealing with something common, such as an ulcer, irritable bowel syndrome, or gallbladder problems. The doctor then often recommends treatments that include dietary changes, the use of an antacid, or even an endoscopy, but they don’t immediately test for pancreatic cancer.
Only after the patient derives no relief and visits the doctor multiple times over the course of several months, is a CT scan ordered. By that time, the symptoms may have progressed to include jaundice, back pain, and weight loss, which means that the cancer is already in the later stages and may have spread to other parts of the body.
For the patient who is eventually being diagnosed with pancreatic cancer, the months that were spent ruling out other diagnoses could mean the difference between life and death.
It is not realistic, or even medically sound, to expect that doctors will approach every patient who complains of abdominal symptoms as if they may have pancreatic cancer.
This is the reason that researchers are now working on finding new ways to test for pancreatic cancer, specifically a non-invasive blood test, which will lead to earlier diagnosis of this cancer and improve the likelihood of survival for patients.
Risk Factors
I am currently leading a clinical trial at the Western Connecticut Health Network with the goal of developing a screening test for people who are at high risk for pancreatic cancer. The traditional risk factors for pancreatic cancer in those without a family history of the disease include obesity, alcohol use, and smoking. But the most notable and only recently recognized risk factor is the development of “new-onset diabetes,” which means people who are at least age 50 and have been diagnosed with diabetes in the past year.
Typically, if new-onset diabetes is caused by pancreatic cancer, the person will be diagnosed with pancreatic cancer within 1 or 2 years after the diagnosis of diabetes. This doesn’t mean that everybody with new-onset diabetes needs to be concerned about pancreatic cancer—they don’t—but we believe that there is a link in some people, and we are studying this link to understand this connection.
Our study involves only people with new-onset diabetes, and our goal is to figure out which patients with diabetes will eventually have pancreatic cancer. If we can figure this out, we may be able to have a new screening test for pancreatic cancer.
Looking for Biomarkers
In this study, we collect blood samples from all study participants every 6 months, and each participant undergoes an MRI annually, with the goal of finding potential indicators of early pancreatic cancer.
Once we have a group of patients with diabetes who later had pancreatic cancer that we are able to catch early, we will then study their blood samples for specific biomarkers (biologic signs) that indicate pancreatic cancer. When we are able to identify biomarkers specific to pancreatic cancer, a blood test can then be used to identify this cancer early in patients who are at risk.
It will take thousands of people before we have enough information to develop this blood test, but it’s a start. My hope is that we could complete the study in 3 years, but much of this will depend on patient involvement. (For more information on this study, visit https://clinicaltrials.gov/ct2/show/NCT03250078.
Current Treatments
Catching pancreatic cancer early could potentially stop the upward trend in deaths from this deadly disease, because the effective treatment options for patients with advanced disease are currently very limited.
When caught early, patients undergo a Whipple procedure (pancreaticoduodenectomy), which removes tumors in the pancreas. More patients receive chemotherapy before the procedure, especially if the tumor is large. Chemotherapy can potentially shrink the size of the tumor, which creates a better situation for the removal of the tumor. In addition, when chemotherapy is given beforehand, it could convert a tumor that may not qualify for surgery into one that can be removed surgically. In some cases, radiation is also administered to enable the removal of the tumor by surgery.
After surgery, patients are typically treated with FOLFIRINOX, a combination of several chemotherapies (fluorouracil, irinotecan, and oxaliplatin) plus leucovorin, for 6 months. FOLFIRINOX is also used in patients with metastatic disease has spread to other parts of the body, such as the liver, lymph nodes, or the abdominal cavity. The other chemotherapy option is a 2-drug combination with Gemzar (gemcitabine) and Abraxane (nab-paclitaxel).
About one-third (33%) of patients with pancreatic cancer who receive chemotherapy for advanced cancer will have a 50% reduction in their tumors. About 50% will have clinical benefit from chemotherapy, meaning that their cancer becomes stable and stops growing, and the patients will feel better.
Feeling better is important, because many of these patients are losing weight and are in pain before treatment. An effective chemotherapy can reverse that, so although they have to deal with the side effects of chemotherapy, it is often outweighed by reducing the cancer burden on the body.
However, overall, the survival for patients with advanced pancreatic cancer is usually less than 1 year.
On the Horizon
Immunotherapies have shown tremendous advancements in the treatment of many cancers, such as lung, kidney, bladder, melanoma, and certain types of colon cancer, but not in pancreatic cancer. Immunotherapy drugs such as Keytruda (pembrolizumab) and Opdivo (nivolumab) have had a major impact on so many cancers, but they have not proved effective in pancreatic cancer, and researchers are not sure why.
We believe that pancreatic cancer itself must be doing something to paralyze the immune system, so that immunotherapy is not able to fight it as in other cancers.
However, a new targeted therapy has shown good results for patients with metastatic pancreatic cancer that is associated with the BRCA gene mutation. In a new study, the targeted therapy Lynparza (olaparib) has shown the potential to delay disease progression. New results from the phase 3 clinical trial POLO were presented in June 2019 at the American Society of Clinical Oncology annual meeting and were published in the New England Journal of Medicine.2
Lynparza is a PARP inhibitor that is already approved by the FDA for the treatment of breast cancer and ovarian cancer in patients with the BRCA mutation. When used as maintenance therapy in patients with pancreatic cancer and a BRCA mutation, Lynparza delayed the progression of pancreatic cancer by 7.3 months versus 3.8 months with placebo.
About 5% of patients with pancreatic cancer have the BRCA mutation. In this study, patients with the BRCA mutation were able to stop chemotherapy after about 4 months and just use this pill to control the disease progression for a period. Although 5% of patients may seem small, this advance can make a big difference for those affected.
References
- National Cancer Institute. Cancer Stat Facts: Pancreatic Cancer. https://seer.cancer.gov/statfacts/html/pancreas.html.
- Golan T, Hammel P, Reni M, et al. Maintenance olaparib for germline BRCA-mutated metastatic pancreatic cancer. New England Journal of Medicine. 2019;381(4):317-327.
Key Points
- The cure rate for early-stage pancreatic cancer is about 20%, but at advanced disease (stage IV), the stage that Alex Trebek is facing, the cure rate is very small
- The key to fighting pancreatic cancer is early diagnosis, but this is still in the research stages
- The reason is that early-stage pancreatic cancer does not have symptoms, although the development of diabetes in adults may be an early sign
- Many researchers are working on developing a blood test to screen for pancreatic cancer
- Lynparza has recently shown promise for patients with metastatic pancreatic cancer and a BRCA mutation
Patient Resources
A Pancreatic Cancer Screening Study in High Risk Individuals
https://clinicaltrials.gov/ct2/show/NCT03250078
National Pancreatic Cancer Foundation
www.npcf.us
Pancreatic Cancer Action Network
www.pancan.org