The days leading up to your first chemotherapy appointment can be filled with stress and anxiety, but with a little preparation you may be able to reduce your stress, increase your understanding, and attain a sense of empowerment. As an oncology nurse navigator with experience in chemotherapy infusion, I’d like to share my tips with you.
#1 Educate Yourself
Ask if your healthcare institution offers a chemotherapy education class. Often the clinic will have a nurse, navigator, or advanced practitioner provide education on the basics of chemotherapy as well as more detailed information (drug name, length of treatment, and expected side effects) on your specific chemotherapy regimen. Your attendance will help you understand how chemotherapy works, the effects it has on the body, and what to expect with your prescribed treatment.
Two sets of ears are better than one, so I would encourage you to bring a support person with you to the class. Some clinics will also provide a tour of the clinic where you’ll receive treatment, which may help to alleviate some of the anxiety you might be feeling about your upcoming treatment.
Some questions to ask about your chemotherapy regimen:
- How will I receive the chemotherapy (oral, intravenous, topical, injection, etc)?
- How often will I receive chemotherapy, and (for intravenous infusions) how long will each treatment take?
- What are the expected side effects?
- If I experience side effects, when and to whom should I report them?
- What are some ways I can help manage or prevent some of the expected side effects?
- How should I prepare prior to my first appointment?
#2 Organize and Prioritize
Staying organized while going through cancer treatment can alleviate some of the stress you may feel. One strategy is to keep a chemotherapy cycle calendar that clearly shows your appointments, a side effect tracker, and contact information for your medical team. Ask your chemotherapy nurse to assist you in setting up your calendar to accurately reflect your treatment regimen.
Depending on the type of chemotherapy you receive, you may need to rearrange your schedule to prepare for “chemo days” and/or “rest days.” On some days throughout your treatment cycle, you will have more energy and be more productive, while on other days you may experience fatigue and side effects that limit your productivity. Arranging your work schedule and home responsibilities to accommodate your treatment schedule can help facilitate a sense of normalcy.
A supportive work environment can be beneficial and potentially remove barriers to your cancer care. I encourage you to share your treatment plan and outline work expectations with your place of employment prior to starting treatment. Your human resources representative will work with you on any necessary accommodations, such as completing disability paperwork, arranging for time off, or taking advantage of the Family Medical Leave Act.
To learn more about your legal rights in the workplace and how to thrive at work while living with cancer, visit Cancer and Careers at cancerandcareers.org.
#3 Understand Your Financial Options
Cancer care can be expensive. Asking for a financial navigator or insurance coordinator up front may alleviate some financial burden and set you up for success. The medical oncology office should have a point person you can speak with regarding your insurance plan and coverage, financial expectations throughout treatment, your monetary responsibility, and payment plan options. You can also inquire if there is any financial assistance available through the clinic or other programs, if needed. The pharmacy can also potentially provide financial assistance or explain discount programs for certain medications.
Cancer care can be expensive. Asking for a financial navigator or insurance coordinator up front may alleviate some financial burden and set you up for success.
It is important to ask for a financial coordinator at each healthcare facility you visit throughout your entire treatment (surgery, radiation, chemotherapy, etc) not just for the medical oncology office, as they are different for each specialist.
You can also contact your insurance company and request a case manager who can provide insurance assistance throughout your treatment journey. This will help you have a direct contact and limit the retelling of your situation when any insurance issues or questions arise.
#4 Utilize Your Village
Going through cancer and cancer treatment can be a daunting task. Life doesn’t stop when you are diagnosed with cancer, which is why having a stable support system is paramount. It is important to identify the people in your support system and to bring someone with you for support when you can. Your support system should comprise positive, reliable people.
On the Day of Chemotherapy
- Bring your village (support person)
- Show up hydrated and arrive early
- Dress comfortably (wear comfortable clothing including stretchy attire to allow for the nurse to reach your IV access (PICC/Port)
- Bring comfort items and activities to pass the time
- Bring anti-nausea medications
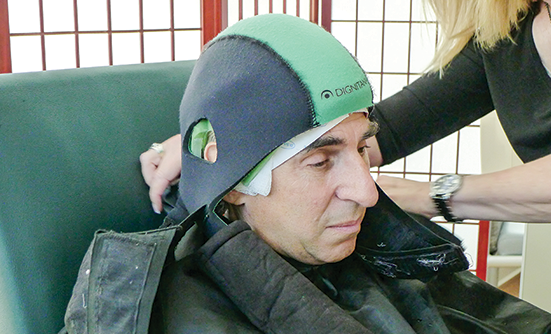
- Bring scalp cooling equipment if appropriate
On the Day of Chemotherapy
- Bring your village (support person)
- Show up hydrated and arrive early
- Dress comfortably (wear comfortable clothing including stretchy attire to allow for the nurse to reach your IV access (PICC/Port)
- Bring comfort items and activities to pass the time
- Bring anti-nausea medications
- Bring scalp cooling equipment if appropriate
Ask the nurse at the infusion center about their visitor policy prior to your first chemotherapy appointment. If you feel comfortable and visitors are allowed, bring a support person to your infusion appointment—someone who can provide emotional support and an extra pair of ears for listening to important information and educational explanations, and who can drive you home when you aren’t able to drive yourself.
Often family and friends want to help you in a meaningful way but are unsure how. It is okay for you to give them actionable recommendations on how best to help you as you move through this journey. If you need help with meals, childcare, or house chores, allow them to assist. For example, asking a loved one if they can pick up groceries for the week or pick your kids up from school are tangible tasks they can do that will take pressure off you. Once you begin treatment, you will start to understand when you will need rest days (days you are more fatigued and/or have more side effects, such as nausea) and when you are able to do your normal activities. Choose your rest days as the days you ask for additional help from your support system. If there is ever a time to ask for help, it is now. Give yourself permission to accept help and lean on those around you.
#5 Know Your Numbers
While receiving any type of chemotherapy, it is imperative to have access to contact information for your oncology team. Usually, the facility will have a 24/7 hotline number for patients to call after hours in case of an emergency. Putting this number in your smartphone, wallet, or on the fridge are some ways you can save this information. It is important that this number is readily accessible in case you need it.
I encourage you to keep your medical team’s contact information readily accessible throughout your treatment journey. Know whom to call and when to call for emergency symptoms, side effect issues, prescription refills, oral chemotherapy questions, and psychosocial support needs.
Know whom to call and when to call for emergency symptoms, side effect issues, prescription refills, oral chemotherapy questions, and psychosocial support needs.
When in doubt, call your navigator who can assist with coordination of care and managing communication among your entire medical team.
#6 Track Your Treatment and Side Effects
Understanding how your specific treatment regimen will affect your body and the expected side effects is crucial to successful side effect management. Not everyone reacts in the same way to medications, and chemotherapy is no different. Your experience may also vary with each treatment; sometimes you may have only 1 or 2 side effects; other times you may have all of them. Preparing and monitoring for all side effects can assist you and your medical team in managing symptoms. Keeping track of your treatment cycles and including notes about side effects—when you experience them, the level of distress they are causing, and what supportive management works to alleviate them—provide important information for your medical team. Including severe and emergency side effects, know what to monitor, when to report it, and to whom to report.
Your medical team cannot address your side effects if they are not informed of them. Patients can sometimes worry about informing their medical team about their side effects for many different reasons, including fear of pausing treatment or feeling like a burden. There are many different options to address and alleviate chemotherapy side effects, so don’t hesitate to discuss them with your medical team so they can find the best option for you. I encourage you to be your own best advocate and not suffer in silence. Speak up and actively engage with your medical team.
It’s important to pick up any prescribed medications (for example, anti-nausea medications) prior to your first treatment and have them readily available.
#7 Plan for a Chemo Day
Every chemotherapy regimen is different and that includes the amount of time the treatment will take. Depending on the type of treatment you are to receive (drug type, route of administration, dose, etc), some chemotherapy treatments can last many hours. Often you will have your blood drawn prior to receiving the drug to confirm your labs are within normal values. You may also receive medications prior to receiving the chemotherapy to prevent potential hypersensitivity reactions or side effects.
The medical oncologist may want to visit with you prior to your first treatment to make sure all your questions are answered as well as to confirm all insurance paperwork and informed consent documents are in place.
I recommend you plan for a total chemo day, meaning, do not plan anything else for that day (work, other appointments, picking kids up from school, etc). The first day of your first treatment may last longer than subsequent treatment; you will be monitored very closely during this first treatment for unexpected reactions to the medication, and you can’t predict how you will feel after treatment.
At-Home Chemotherapy
Planning for a chemo day with potential side effects should be considered for all types of chemotherapy (oral, topical, at home) not just for therapy completed in a clinic. For oral and/or at-home chemotherapy, you will still need to plan your days around side effects and how you feel. You will also need to be informed on how to manage and safely handle the chemotherapy, when to take it, and what to take it with, as well as expected side effects and what to monitor and report to your healthcare professional.
About the Author
Jordan Henderson is director of program development for the Academy of Oncology Nurse & Patient Navigators. She is an oncology certified nurse and certified navigator with experience in chemotherapy infusion, breast cancer navigation, and survivorship navigation program development. As a strong patient and navigation advocate, she currently works with AONN+ to enhance and build meaningful programs that serve navigators, patients, and caregivers.
You Might Also Like
Is It Possible to Prevent Hair Loss?What you should know about scalp cooling before starting chemotherapy.